 
Malunion, however, is not uncommon, and can lead to residual pain, grip weakness, reduced range of motion (especially rotation), and persistent deformity. Nonunion is rare almost all of these fractures heal. Very rarely, pressure on the muscle components of the hand or forearm is sufficient to create a compartment syndrome which can manifest as severe pain and sensory deficits in the hand. Swelling and displacement can cause compression on the median nerve which results in acute carpal tunnel syndrome and requires prompt treatment. Decreased sensation especially at the tips of the radial three and one half digits ( thumb, index finger, middle finger and radial portion of the ring finger ) can be due to median nerve injury. Tenderness at an area with no obvious deformity may still point to underlying fractures. Examination should also rule out a skin wound which might suggest an open fracture, usually at the side. The wrist may be radially deviated due to shortening of the radius bone. Reverse deformity is seen in volar angulation ( Smith's fracture). "Dinner fork" deformity of the wrist is caused by dorsal displacement of the carpal bones ( Colle's fracture). Swelling, deformity, tenderness, and loss of wrist motion are normal features on examination of a person with a distal radius fracture. Any pain in the limb of the same side should also be investigated to exclude associated injuries to the same limb. Any numbness should be asked to exclude median and ulnar nerve injuries. People usually present with a history of falling on an outstretched hand and complaint of pain and swelling around the wrist, sometimes with deformity around the wrist. Most children with a buckle wrist fracture experience a broken wrist for life and do have an increased chance of re-fracturing the same spot or other adverse effects. A year or two may be required for healing to occur. Distal radius fractures represent between 25% and 50% of all broken bones and occur most commonly in young males and older females. ĭistal radius fractures are common, and are the most common type of fractures that are seen in children. Among those who are cast, repeated X-rays are recommended within three weeks to verify that a good position is maintained. 
Surgery is generally indicated if the joint surface is broken and does not line up, the radius is overly short, or the joint surface of the radius is tilted more than 10% backwards. 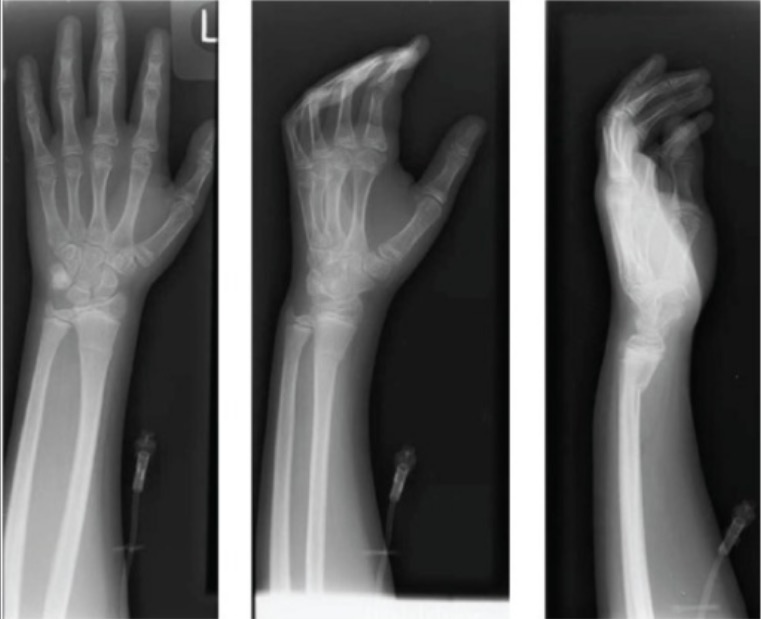
Treatment is with casting for six weeks or surgery. The diagnosis is generally suspected based on symptoms and confirmed with X-rays. Specific types include Colles, Smith, Barton, and Chauffeur's fractures. In older people, the most common cause is falling on an outstretched hand. In younger people, these fractures typically occur during sports or a motor vehicle collision. Symptoms include pain, bruising, and rapid-onset swelling. Pain, bruising, and swelling of the wrist Ĭolles' fracture, Smith's fracture, Barton's fracture, Hutchinson fracture Ī distal radius fracture, also known as wrist fracture, is a break of the part of the radius bone which is close to the wrist. Treatment of radial head fractures depends on the specific characteristics of the fracture using the Mason classification.A Colles fracture as seen on X-ray: It is a type of distal radius fracture. Radial head fractures may be difficult to visualize on initial imaging but should be suspected when there are limitations of elbow extension and supination following trauma. Combined fractures involving both the ulna and radius generally require surgical correction. These fractures are treated with immobilization or surgery, depending on the degree of displacement and angulation. Isolated midshaft ulna (nightstick) fractures are often caused by a direct blow to the forearm. It should be noted that these fractures may be complicated by a median nerve injury. A nondisplaced, or minimally displaced, distal radius fracture is initially treated with a sugar-tong splint, followed by a short-arm cast for a minimum of three weeks. In adults, distal radius fractures are the most common forearm fractures and are typically caused by a fall onto an outstretched hand. Depending on the degree of angulation, buckle and greenstick fractures can be managed with immobilization. Greenstick fractures, which have cortical disruption, are also common in children. Incomplete compression fractures without cortical disruption, called buckle (torus) fractures, are common in children. If initial imaging findings are negative and suspicion of fracture remains, splinting and repeat radiography in seven to 14 days should be performed. Evaluation with radiography or ultrasonography usually can confirm the diagnosis. A fall onto an outstretched hand is the most common mechanism of injury for fractures of the radius and ulna. Fractures of the radius and ulna are the most common fractures of the upper extremity, with distal fractures occurring more often than proximal fractures. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
